Total Knee Replacement
FAQ
Total Knee replacement Video
Introduction
What causes a painful knee?
When one or more parts of the knee are damaged it can become painful and movement becomes restricted. Over time, cartilage (the smooth covering at the ends of the bone in the joint) can crack or wear away. When this happens, the bones making up the joint rub together.
No matter your age, a knee problem may keep you from activities you enjoy. Pain and stiffness may even limit your day-to-day activities. Problems with the knee joint tend to build up over time.
Any of the problems below may lead to joint damage and hence knee pain:
OSTEOARTHRITIS
As time goes by, normal wear and tear can add up. Cartilage may begin to wear away (osteoarthritis). As the bones rub together, they become rough and pitted. Previous meniscectomies and damage to the anterior cruciate ligament inevitably lead to osteoarthritis.
INFLAMMATORY ARTHRITIS
This is a group of conditions where the lining of the joint becomes inflamed and secretes material that destroys the joint cartilage. In these conditions more than one joint is usually affected. The joints are hot, swollen, painful and deformity is common.
AVASCULAR NECROSIS
This can occur for no reason (idiopathic) or can be secondary to a number of conditions (e.g. long-term use of alcohol or steroids). It is due to loss of blood supply to the bone. If the bone dies (necrosis), the joint will become arthritic. This pain often comes on quite suddenly and may increase rapidly. This can happen at any age. There are many other causes of this condition but they are rare.
FRACTURE
A bad fall or blow can break (fracture) the bone. If the broken bone does not heal properly the joint may wear down like a tyre that is not balanced.
LIGAMENT INJURY
Injuries to ligaments causing instability of the knee can and usually do lead to premature arthritis.
CHILDHOOD KNEE PROBLEMS
Occasionally knee pain results from a problem which may have started in childhood such as osteochondritis dissecans, trauma, and juvenile rheumatoid arthritis. Note: Osgood-Schlatter disease does not cause arthritis.
INFECTION
Infection can destroy the cartilage lining, leading to osteoarthritis.
OTHER CAUSES
- A bad injury that did not heal properly
- Obesity
- Long term exposure to sports or heavy manual labor
- Long term high intensity, high mileage running (controversial)
- Other rare diseases affecting bones or soft tissue causing severe pain in the knee and may lead to arthritis.
What is a knee replacement?
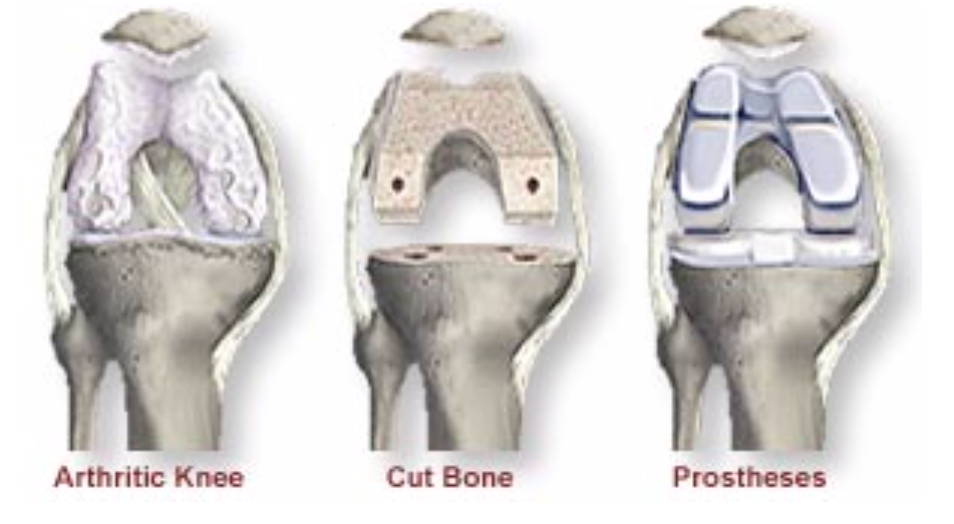
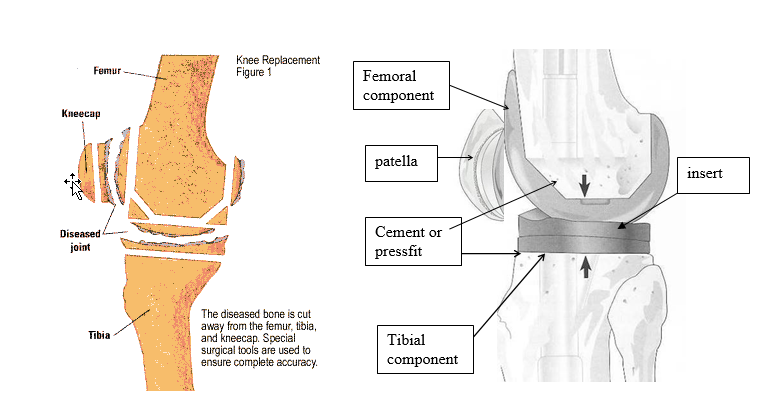
Total knee replacement became popular during the 1970’s. Since then it has become a very common procedure but advances are continuing to be made. The aim of the operation is to replace the bottom end of the femur and the top end of the tibia with a man-made device (prosthesis). The back surface of the patella is also commonly resurfaced. These devices are combinations of metal, plastic and sometimes ceramic materials. They are fixed to the bone either using bone cement or by using a prosthesis with a rough surface. This relies on your bone growing onto the implant for long term stability. It may be reinforced with screws on the tibial side. In between the two components is a special plastic liner made out of polyethylene. This has a curved surface and may actually move in some knee designs. The polyethylene is the part of the knee which often wears out over time and may need to be changed.
Total knee replacement is not a complete solution to the problem as they become loose with time and may need to be revised (which means another operation) within ten to fifteen years. Your surgeon chooses the best prosthesis for your particular problem and decides whether a cemented or non-cemented technique will be used.
Benefits
You do not have to live with a painful knee for the rest of your life. During this surgery your problem knee joint is replaced with an artificial joint (a prosthesis). After a total knee replacement, you can look forward to moving more easily and without pain. Most people gain all the following benefits:
- Stops or greatly reduces knee pain. Even the pain from surgery should go away within weeks.
- Increased leg strength. Without knee pain you will be able to use your legs more and build up your muscles.
- Improves quality of life by allowing you to do activities of daily living and low impact activities in greater comfort.
- Enables you to sleep without pain.
- Provides years of reliable function. Most total knee replacements last for many years.
When should you have a knee replacement?
When you have arthritis on your x-ray and pain and stiffness from your knee joint cause:
- Severe disability
- Stops you or makes it difficult to perform your job
- Interferes with your leisure activities
- Interferes with your walking or mobility
- Wakes you at night despite non-operative treatment such as drugs
- When conservative treatment such as analgesia, anti-inflammatories, weight loss, physiotherapy
and aids like crutches or a cane has failed
Remember it is an elective procedure and should only be performed when you are no longer prepared to put up with your pain and disability, and understand the benefits versus the risks involved.
Pre-Operation
Pre-Admission Clinic
You will usually be required to attend a pre-admission clinic and/or see a physician prior to your surgery and have some simple tests. The tests required are:
- Blood tests to ensure your blood count is normal and you have no other major medical problems.
- ECG, wherein a Cardiograph of your heart will be taken to make sure you have no underlying cardiac problems.
- X-rays. Always bring x-rays of your knee to hospital. Dr Walker may or may not require new x-rays of the knee he is operating on.
- Urine sample is required to ensure you do not have a urinary tract infection. An infection anywhere before surgery (e.g. infected toenail, skin lesion, throat infection, gum or dental infection) can greatly increase your chances of infection of the joint replacement following surgery. If an infection is found, it will be treated with simple antibiotics prior to surgery.
All relevant information about what to do before, during and after your stay in hospital will be discussed at length at this clinic.
Medications
- 10 days prior to surgery, cease aspirin and anti-inflammatory medications (e.g. Voltaren, Feldene) as they may cause bleeding
- 10 days prior to surgery cease any naturopathic or herbal medications as these may also cause bleeding
- Continue with all other medications unless otherwise specified
Home Preparation
- Arrange for someone to help out with everyday tasks like cooking, shopping and laundry
- Put items that you use often within easy reach before surgery so you won’t have to reach and bend as often
- Remove all loose carpets and tape down electrical cords to avoid falls. Make sure you have a stable chair with a firm seat cushion, a firm back and two arms
- Make sure your shower or bath is safe and easy to get in and out of. Handrails, non-slip mats and suitable stools to sit on are helpful for personal safety and comfort
Other
- Notify Dr Walker if you have any abrasions, cuts or pimples around the knee
- Bring any X-rays, MRI scans or other relevant investigations you have had done to your surgery
- You are advised to stop smoking for as long as possible prior to surgery.
Procedure
- The anaesthetist will see you before the surgery wherein, they will discuss with you if they are going to do a spinal or general anaesthetic
- You are taken to the operating theatre and while you are still awake, you are placed on the operating table and set up for surgery with a tourniquet placed around your thigh.
- A urinary catheter will be placed in your bladder to measure your fluid balance during and after surgery.
- A cut is made in the skin and underlying tissues to expose the knee.
- Special instruments are used to make very accurate cuts in the bone to fit the prosthesis.
- Trial components are put in first to make sure everything fits properly.
- The bone is then cleaned to remove debris.
- The real components are then inserted with or without cement.
- Drains are usually inserted.
- The wound is then carefully closed in layers, the last being the skin.
- A dressing is applied and you are taken to recovery.
Post-Operation
After Your Operation
- Your leg will be bandaged from groin to toes.
- Your fluid input and output are measured carefully. A drip in the arm will be used to give you fluid, replace blood during the operation and for antibiotics.
- Pain is normal after the operation but if your pain is not reduced be sure to tell the nurse. Pain medication may be injected into a muscle or delivered by IV into the blood stream.
- The drip, drains and catheter are removed on your surgeon’s advice at approximately 24 hours after surgery.
- Blood will be taken 24 to 48 hours after the operation to check your haemoglobin and blood chemicals.
- Your exercise regime will begin as soon as you are capable and this will continue during your stay in hospital and once you are at home. This will be supervised by a physiotherapist.
- You will be discharged 2-5 days post-operatively depending on your progress. In some cases you will be sent to a rehabilitation centre before you go home to have hydrotherapy and physiotherapy.
- Sutures are usually dissolvable but if not, are removed at about 10 days.
Recovery
- You are in hospital approximately 5 days. At Day1 or 2 you will get up on a frame and then you progress to crutches and then a stick usually by 4 – 6 weeks.
- If you go to rehabilitation, you are generally in rehab for 1 – 2 weeks. This will include aggressive physiotherapy and hydrotherapy.
- When you leave hospital, you will probably still require tablets for pain but no injections. Wean your medications down to Panadol as soon as possible.
- It is best to avoid anti-inflammatories if you have arthritis elsewhere for 1 week to avoid any possible bleeding. You lose 60 – 80% of your pain by six weeks and 95% of your pain by 12 weeks. By 12 weeks you can usually walk as far as you want to.
- Regaining movement early is extremely important. Getting the knee straight is as important as bending. Do not put anything under the knee even though it feels comfortable, as it prevents it from straightening.
- You can drive when you have regained muscle control, usually by 6 weeks.
- People can usually return to work somewhere from 8 – 12 weeks. Heavy manual work may take longer.
- Normally by 3 months you can play sports like golf, bowls, stationary bike ride, bush walk, doubles tennis and swim.
Results
This operation is generally very successful. It is an excellent procedure to improve a person’s quality of life. After this operation 95% of people are good or excellent. Good means occasional aches and pains which do not require painkillers and excellent means no significant pain or discomfort. There are some people who will have unexplained pain.
In general, 90 – 95% of knee replacements survive 15 years but this depends on a number of variables such as your age and activity level. Here we use the analogy of a tyre. The more you drive on it, the quicker it wears out. The better it is looked after and serviced, the longer it will last.
Special Precautions to Take
- Remember this is an artificial knee and must be treated with care.
- In general, the more active you are doing the quicker your knee will wear out.
- Avoid situations where you might fall.
- Your knee may go off in a metal detector at the airport. You can receive a note from the doctor’s rooms to say you have had a joint replacement.
- Prevention of infection is vital. If you have any infections anywhere, make sure you see your local doctor straight away for treatment. If you get increasing pain in your joint, are sick and have a temperature you should go to hospital to get checked out.
Antibiotics should be prescribed if you have an infection anywhere in the body, if you have surgery in contaminated areas such as teeth, nose, bowel or bladder, podiatry treatment or urinary catheterisation.
Activities Post-Surgery
- You should avoid placing excess stress on the joint, this may occur through ‘pounding activities.’
- Walking is good.
- Swimming in a pool or light surf between the flags is safe.
- Doubles tennis is allowable but anything more aggressive will lead to premature wear of your joint. Contact sports are prohibited and jogging can be detrimental to the long-term survival of your joint replacement.
- Skiing on groomed slopes if you are a good skier is acceptable as long as you are aware you can cause significant damage if you fall.
- Bowls and golf should not be a problem.
Risks and Complications
Any operation, big or small, has risks. The following can occur with any surgery and some rarer complications may also be possible. The utmost care is taken at all times during surgery to prevent these complications. Dr Walker is a subspecialist and operates within his defined area of expertise. This minimises the risk of complications.
You will need to sign a consent form prior to your surgery stating that you understand these risks and wish to go ahead with the surgery. Complications can be related to the anaesthetic or general in nature.
Some complications specific to total knee replacement are:
- Infection
- Fracture
- Stiffness
- Damage to nerves or blood vessels
- Blood clots
- Wound irritation or breakdown
- Wear
- Osteolysis
- Damage to ligaments
- Dislocation
- Heterotopic ossification
- Cosmetic appearance
- Leg length inequality
- Breakage of the implant
The above list is not exhaustive. For more information on complications:
Total Knee Replacement Complications
Frequently Asked Questions
What is the prosthesis made of?
These devices are combinations of metal and plastic and sometimes ceramic materials.
What is used to attach it to my bones?
They are fixed to the bone either using bone cement or by using a prosthesis with a rough surface, which relies on your bone growing on to the implant for long term stability. It may be reinforced with screws on the tibial side. In between the two components is a special plastic liner made out of polyethylene.
When can I go back to work?
Most patients return to sedentary jobs at 3-6 months after total knee replacement. It must be stressed to the patient before surgery that they may not return to manual labour after joint replacement. Any heavy manual job will result in premature loosening of the joint replacement and pain due to the increased stress on the joint replacement. Clerical or supervisory duties are suitable for a patient with a total knee replacement.
When will I be able to drive again?
When you feel comfortable using your leg fully. For most people, they feel comfortable driving after six weeks. Please also check with your insurance company as they may have specific rules on when you can drive after surgery.
When will I be able to resume sexual intercourse?
Sexual intercourse is allowed when the patient is comfortable but they have to be in charge of the positions used and any significant discomfort should result in the patient abstaining until they talk to their doctor.
In general, sexual intercourse occurs at around three to six weeks post operatively.
When will I be able to play sports?
Obviously, pounding sports are not good for joint replacement as they can wear the articulation. We recommend walking, bushwalking, swimming, stationary bike riding, doubles tennis and skiing on groomed runs if the patient is already a good skier. Jogging and heavy weights, although possible, will wear the joint prematurely.
